Neuroendocrinology of stress
It is obvious that the higher cortical functions must exercise some effect on the mediation of stress. The best example of this is Wolff's description of unconditional (direct stressors)and conditional (indirect stressors/ie symbols). In both situations the GAS is activated. To understand this activation we must understand the hypothalamic-pituitary system.
Hypothalamic-pituitary-adrenal system
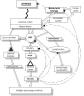
As you recall the pitiutary has two parts, the anterior and posterior hypophysis. It is connected to the hypothalamus via a portal vessel system. Releasing factors corticotrophin releasing hormone, (CRH) and thyrotropin releasing hormone, (TRH) and inhibitory factors such as prolactin inhibiting factor (PIF) from the hypothalamus enter this portal system and arrive in the adenohypophysis (anterior pituitary) and cause the release of pituitary hormones. In stress there is a vigorous release of CRH (CRF is the same molecule) centrally by the hypothalamus. CRH causes a release of ACTH by the pituitary. ACTH which enters the venous blood and on arrival at the adrenal cortex causes a stimulation of the synthesis and release of cortisol. The released cortisol goes "everywhere" including the ptiuitary where it inhibits further release of ACTH. In addition there are cortisol receptors in the central nervous system on which the cortisol acts. Some of these receptors inhibit hypothalamic release of CRH. CRH also causes a vigorous medullary secretion of epinephrine and
norepinephrine when given intraventricullarly. This suggest a common pathway for the central transduction of stress onto the adrenal cortex and adrenal medulla.
A significant aspect of the release of ACTH involves its synthesis. ACTH is part of a prohormone, proopiomelanocortin (POMC). In addition to ACTH this hormone is split into MSH (melanocyte stimulating hormone) and beta-endorphin.
Neurotransmitters and HPA
The neural systems which influence the HPA has been studied by various groups. The neurotransmitters acetylcholine and serotonin appear to stimulate ACTH release. Serotonin is produced from tryptophan. In fact the availablitlity of tryptophan is the rate limiting factor for serotonin synthesis. Tryptophan is of interest in stress. This amino acid is carried in the blood stream primarily bound to albumen at the fatty acid site. The uptake into the brain is the result of a facilatated transport system. The free concentration of tryptophan is increased by increased concentration of free fatty acids in the blood. As we mentioned earlier epinephrine and cortisol increase free fatty acids. This increase in availability of tryptophan acts to increase serotonin synthesis. This increase could act as a feed-forward regulatory system because ACTH increases cortisol synthesis. Continued stress would exhaust the tryptophan supply and result in a relative serotonin depletion. The symptoms of serotonin depletion are essentially indistinguishable from clinical depression and include effects on appetite, sleep, concetration, and irritability.
Norepinephrine inhibits ACTH release.
The effects of norepinephrine is complicated by evidence for a norepinephrine alpha receptor stimulatory pathway. It is known is that stress is a strong stimulus for the activation of the locus ceruleus. It is possible that the norepinephrine released acts as a govenor or restraint for the feedforward effects of the serotonin system mentioned above.
GABA causes an inhibition of CRF release.
The antianxiety drugs known as benzodiazepines are GABA agonist. In some models GABA agonist may reduce the chronic stress response. The cost of such treatment is the potential for addiction. In addition it is likely that the anti-stress effect of the benzodiazepines is short-lived and the animal becomes tolerant to the medication.
Neuropeptides such as beta-endorphin and met-enkephalin have been associated with the stress response since their discovery. These neuropeptides have opiate receptor binding ability. Of interest is that beta-endorphin is part of the same pro-hormone which contains the ACTH sequence, POMC. Beta-endorphin and met-enkephalin inhibits ACTH release.
![[Image: attachment.php?aid=8760]](http://www.breastnexus.com/attachment.php?aid=8760)
 http://www.uams.edu/m2004/Behavioral%20S...20text.htm
http://www.uams.edu/m2004/Behavioral%20S...20text.htm




